In 2016, Dr. Rassamee Ling was given the news that all women dread. She had breast cancer. As an anesthesiologist at Surrey Memorial Hospital (SMH), Ling knew more about the diagnosis than most people. It would involve not only surgery but a long and painful recovery. Ling had witnessed the agony that many women suffered after surgery.
“I had a diagnosis of breast cancer, and having been an anesthesiologist for several years, I was dreading the anticipated postoperative pain because I had seen so many other people suffer significantly,” says Ling. She was also aware that poorly controlled pain immediately after surgery increased the risk of developing chronic pain.
Such persistent discomfort is known as post-mastectomy pain syndrome (PMPS). This postoperative complication affects between 20% to 50% of mastectomy patients. The condition leads to chronic pain lasting longer than three months.
A Possible Solution
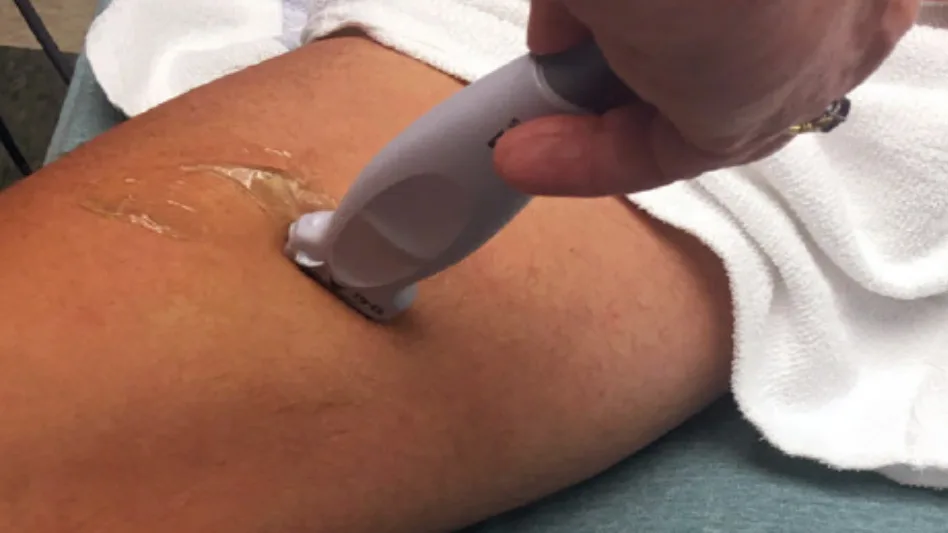
Ling was anxious at the possibility of months of pain. Fortunately, colleagues Dr. Peter Gajecki and Dr. Brenda Lau suggested a solution: a pectoralis nerve block. This ultrasound-guided procedure numbs the nerves in the chest and armpit area and has been shown to reduce acute pain associated with the tissue trauma of a mastectomy. Gajecki learned how to perform the technique by watching a video online and experimenting on himself.
“He’ll forever be my hero,” says Ling. “He practiced on himself the day before my operation and then, on the morning of surgery, showed me his little band-aid and told me that he had great hopes for the nerve block.”
Dr. Lau, Founder and Medical Director of ChangePain clinic also provided additional support. “She shared advice with me when I was a surgical patient in 2016 that proved invaluable,” said Ling.
Ling’s surgery combined an ultrasound-guided nerve block and a general anesthetic. “When I woke up, I was amazingly comfortable, and that comfort and manageable pain allowed me to go home the same day after a major operation,” Ling said.
Ultrasound-guided nerve blocks can relieve pain for up to 24 hours. Dr. Ling says her actual pain control after surgery was 36 hours from the nerve block and then manageable after it wore off.
Launching the Ultrasound Guided Nerve Block Program
After her recovery, Ling was determined to see how ultrasound-guided nerve blocks could help other surgery patients. “I became passionate about expanding our program so every patient would have this.”
Ling followed up on her pledge. Over the next few years, Dr. Ling and her colleagues from the SMH anesthesia department collected data and educated stakeholders on the benefits of ultrasound-guided nerve blocks.
In March 2020, the government of British Columbia halted all non-urgent surgeries. For three months, only emergency surgeries were performed. However, as the first wave of the pandemic began to subside in May 2020, there was a strong push to resume elective surgeries.
The anesthesia department seized this as an opportunity. Dr. Alex Vesely, a member of the executive leadership group, proposed an ultrasound-guided regional anesthesia program for Fraser Health. The physicians knew ultrasound-guided nerve blocks would allow patients to go home quickly after surgery. Fraser Health agreed and in May 2020, they initiated the Block program.
The Impact of Ultrasound-Guided Nerve Blocks on Hospital Stay
The anesthesia department knew ultrasound-guided nerve blocks would benefit the hospital and patients in several ways. They started a trial with knee replacement surgery patients. Patients were given an ultrasound-guided regional anesthetic called an adductor canal block.
“We followed patients on the ward and were thrilled with the results,” says Ling. “We’re finding that instead of staying two or three nights in the hospital, patients often go home the next day if they have no comorbidities.”
Also, since no vaccine was available then, there was a need to limit the risk of infection to operating room staff by avoiding general anesthesia whenever possible as it is considered an aerosol-generating procedure. Joint replacement surgeries could be done with a combination of conscious sedation, spinal anesthesia, and an ultrasound-guided nerve block.
“We had a strong incentive to get patients home faster while there was a shortage of beds in the hospital,” Ling explained.
Lastly, ultrasound-guided nerve blocks increased operating room efficiency, by helping the hospital catch up on canceled elective cases, and with the opioid crisis looming during the pandemic health professionals were able to prescribe less pain medication to patients when they went home.
Today, everyone undergoing knee surgery at Surrey Memorial Hospital gets an ultrasound-guided nerve block. The service has expanded into other surgical services at SMH, and Dr. Vesely credits his colleagues in the Anesthesia Department for the program’s success.
“The block program was born from everyone’s willingness to give more. Staff invested their blood, sweat, and tears to care for our patients and colleagues.”
Nerve Blocks Minimize Post-Surgery Complications
Major operations such as mastectomies and knee replacement surgery require opioids to control patient pain. Some side effects can occur depending on the time these medications are given. One study suggests that up to 50% of patients experience postoperative nausea and vomiting (PONV).
Ultrasound-guided nerve blocks have reduced these post-surgery complications. By lessening the amount of medication needed during and after surgery. This helps to alleviate patients’ pain and make them more comfortable.
Conclusion
With the help of generous donors, the Surrey Hospital Foundation was able to purchase three state-of-the-art ultrasound machines. These machines will enable anesthesiologists to perform nerve blocks with greater precision and accuracy, resulting in better patient outcomes. The Surrey Hospital Foundation is proud to support the Regional Nerve Block Program in its efforts to improve healthcare services in Fraser Health.
Dr. Ling is grateful to the Foundation for supporting the program. “Having good equipment for real-time ultrasound-guided regional anesthesia has been key to perioperative analgesia improvements at SMH. Many thanks to the Foundation from our Department of Anesthesia.”
Additional Resources
Making sure patients are as healthy as possible before their operation can increase the chances of the surgery being successful and lower the risk of complications afterwards. This is called prehabilitation, and it involves optimizing the patient’s health by addressing various risk factors such as nutrition, smoking cessation, and pain management.
Dr. Lau’s Changepain clinic offers a holistic surgical optimization program that ensures patients are ready for surgery by connecting them to a multidisciplinary healthcare team. To learn more about this program, please visit www.changepain.ca.
 About the Author
About the Author
This article is a guest post by Denise Moulton, a registered nurse that works at the Jim Pattison Outpatient Care and Surgery Centre in Surrey. Denise is passionate about writing. Her background in journalism allows her to create compelling and informative content that resonates with anyone interested in healthcare. In her free time, Denise can be found exploring British Columbia’s hiking trails.


